In this article, we explore insulin resistance and pre‑diabetes. While some people use these terms interchangeably, they aren’t quite the same. We’re here to set the record straight and answer key questions about both, read on to learn more.
Does “insulin resistance” mean the same thing as “pre-diabetes”?
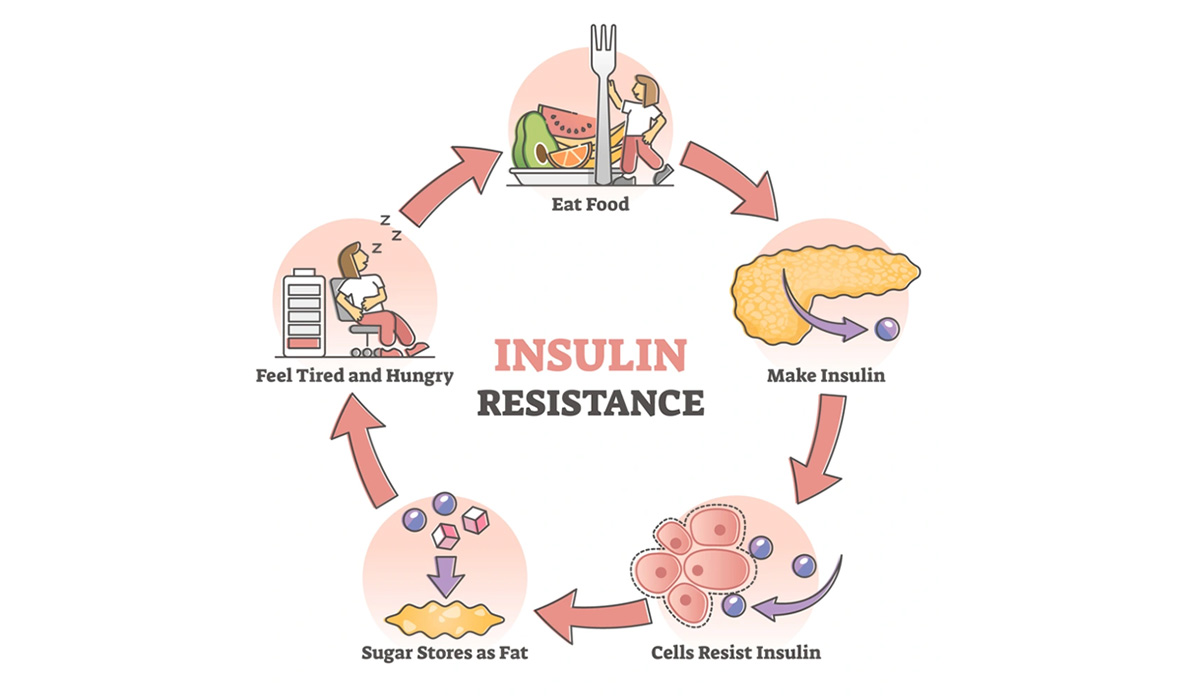
No, these terms are not the same, although they are closely related. Both conditions have problems either using or making insulin in the body. Insulin is the hormone secreted by the pancreas, regulating the glucose that enters the blood stream as food is broken down after eating. After a meal, insulin levels rise to make sure that the right amount of glucose enters the cells in the body.1
The differences between the two conditions
Insulin resistance:
This is the underlying condition where the cells of the muscles, fatty tissue and liver stop responding as well to insulin. These cells can’t take up as much glucose from the blood. Initially the body tries to compensate for insulin resistance by making more insulin to maintain normal blood glucose levels. Over time the pancreas can’t produce enough insulin to overcome insulin resistance. This leads to high blood glucose and the development of pre-diabetes.
Pre-diabetes:
This is defined as the diagnosable state of elevated blood sugar that arises from having insulin resistance. With pre-diabetes you will have higher-than-normal blood glucose but it is not high enough yet to be classified as Type 2 diabetes.
How would you know if you are insulin resistant?
There is no single test to determine if you are insulin resistant and many people have no symptoms. Doctors look at a combination of blood glucose levels, cholesterol levels and physical examination results. Test results may show elevated blood pressure, having a combination of high triglycerides and low HDL cholesterol (this is the good cholesterol), high insulin levels on fasting or after a glucose load and an elevated fasting blood glucose.
A physical sign associated with insulin resistance is the appearance of dark, velvety patches of skin under the armpits, the side and back of the neck and in the groin area. Other signs can be skintags around the neck and in the armpits, acne and oily skin, excess hair growth on the face or the body in females and central obesity (an increased waist circumference or abdominal fat).


















Community