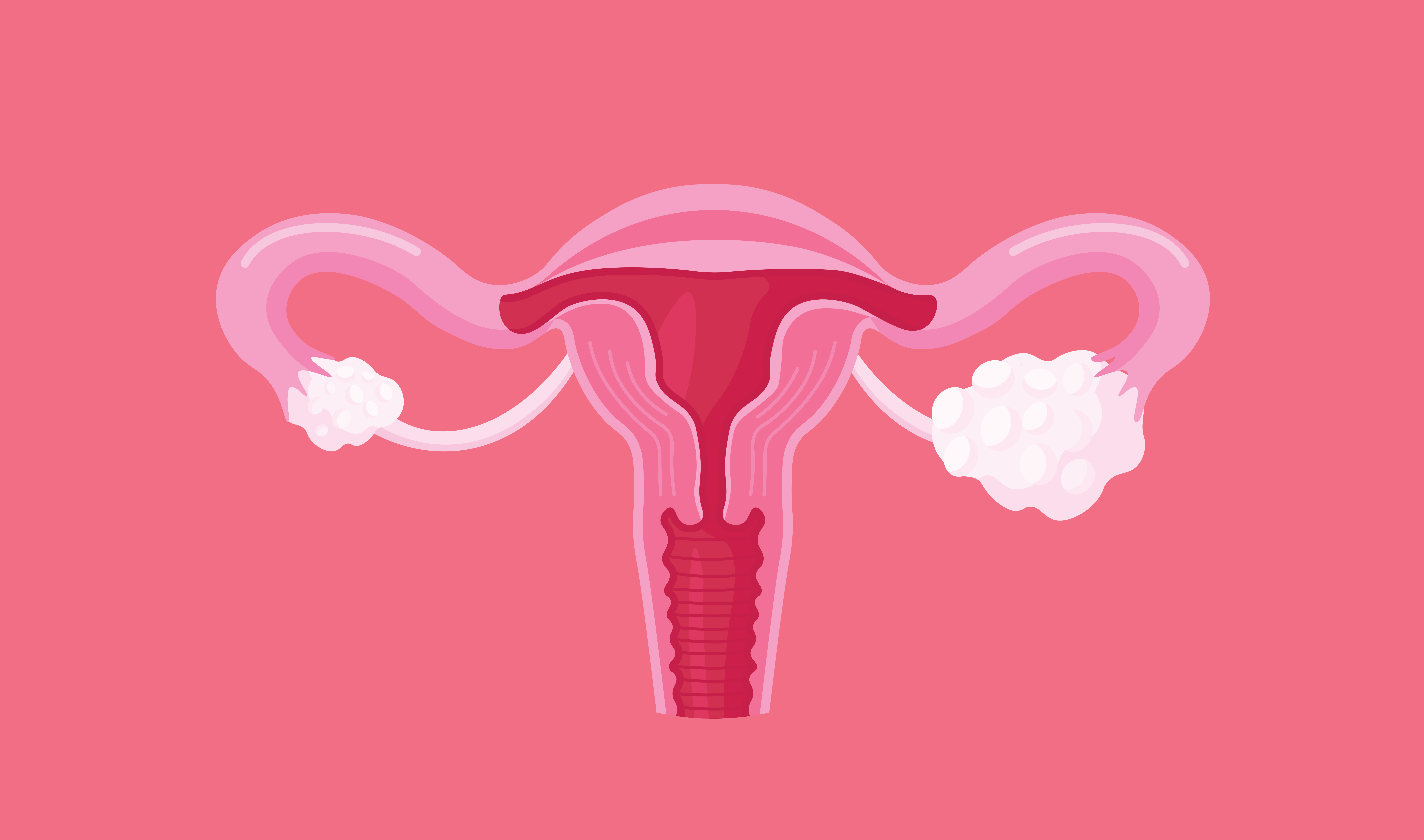
Endo or Endometriosis, is an inflammatory disease that affects about one in ten women. It happens when tissue similar to that found in the uterus lining (endometrium) is found in other places in the body. This tissue still acts the same as when a woman has her period i.e it bleeds with each menstrual cycle into the body causing pain and inflammation.
This tissue can be found in and around the pelvis, bladder, ovaries, fallopian tubes and/or bowel. It has even been found in the lungs.
What Are The Symptoms?
This condition is well-known for the pain it can cause – severe period pain, pelvic pain, pain at ovulation or at other times of the cycle, painful sex, painful bowel motions, painful wind, pain going to the toilet during your period, and/or pain in other places such as the lower back. Other symptoms include sub-fertility and infertility, bowel problems such as bloating, diarrhoea, constipation, bladder troubles (pain before or passing urine, frequent urinary tract infections), abnormal menstrual bleeding, tiredness and low energy. Some women may have endometriosis while having no symptoms at all. Symptoms usually improve during pregnancy and after menopause.
Who Gets Endo?
The exact cause of endometriosis is not known however there seems to be a genetic link as women often have a family history of the disease, usually a mother or sister with the condition.
Endometriosis can often be diagnosed based on a woman’s medical history and her symptoms but may also require physical examinations and scans. However a procedure called laparoscopic surgery is the only definitive way to determine for sure whether a patient has endometriosis. This surgery is done in hospital under general anaesthetic and involves a doctor viewing the pelvic cavity using a camera inserted through a small incision near the belly button. If any adhesions are found these can be removed at the same time. Unfortunately with endometriosis, while it can be treated, it can not be cured, as in many cases endometrial adhesions grow back.
How Can Endo Be Treated?
The treatment for endometriosis depends on how severe your symptoms are, where it is in your body and whether you plan to have children or are finished adding to your family.
Initial medical treatment starts with pain relief medication such as paracetamol and anti-inflammatories like ibuprofen. Some women are prescribed an oral contraceptive pill which can relieve the symptoms of endometriosis if taken continuously. Sometimes intra-uterine devices (IUDs) can be useful to decrease heavy periods and can help to decrease pain.
More invasive treatment such as surgery to remove the ovaries (oopherectomy) can be required if the ovaries have been severely damaged. A hysterectomy (where the uterus is removed) can be advised if pain is severe or long-standing, or if there is extensive endometriosis.
What Can I Do To Alleviate Symptoms?
Self-help treatments are invaluable in treating this condition. Stress and anxiety can make pain worse, so anything that can help to decrease stress and anxiety may help. Regular exercise, massage and physiotherapy can help with this. It is important to look after your diet, especially if suffering from bowel-related symptoms. Try and decrease the following foods and fluids which can irritate the bowel – alcohol, coffee, fizzy drinks, very spicy foods, food with preservatives and additives as well as animal fats in dairy products and processed foods.
Don’t Put Up With Pain, Get Help
Many women associate having periods with having a lot of pain. This should not be the case. You should not put up with severe pain. If you suffer from severe pain with each period, your period pain is getting worse each cycle, or going on the pill to control painful periods has not helped, seek help from your doctor. If you are finding it difficult to get pregnant, also seek medical treatment early. While endometriosis is not a condition that can be cured, it can be effectively treated and managed.
















Community