What is dermatitis?
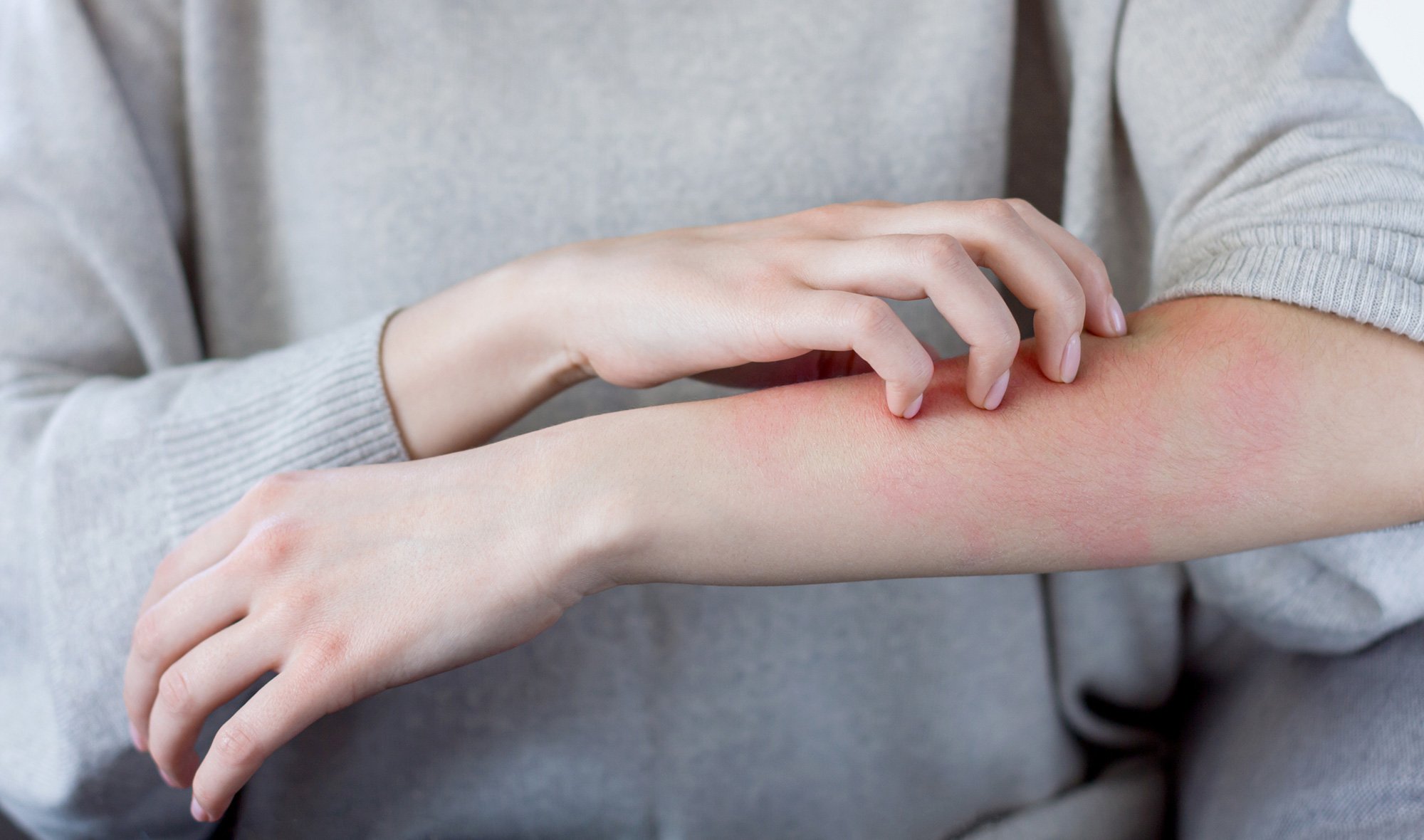
Inflammation of the skin is it’s way of reacting to an irritant or allergen (something that causes an allergic reaction) and can occur anywhere in the body, although it is most common on the face, elbows, wrists, arms and knees, where the skin is at its thinnest.
Causes and triggers
The cause of dermatitis can be obvious as the reaction can be related to a specific substance like perfume, washing powder, a solvent or glue and the reaction is usually restricted to the area of contact. Sometimes the cause is a combination of factors, including genetic inheritance, allergy exacerbated by environmental changes, humidity or temperature. Scratching makes it worse, setting up an itch-scratch-itch cycle because scratching releases histamine, a chemical involved in allergic reactions.
Common forms of dermatitis
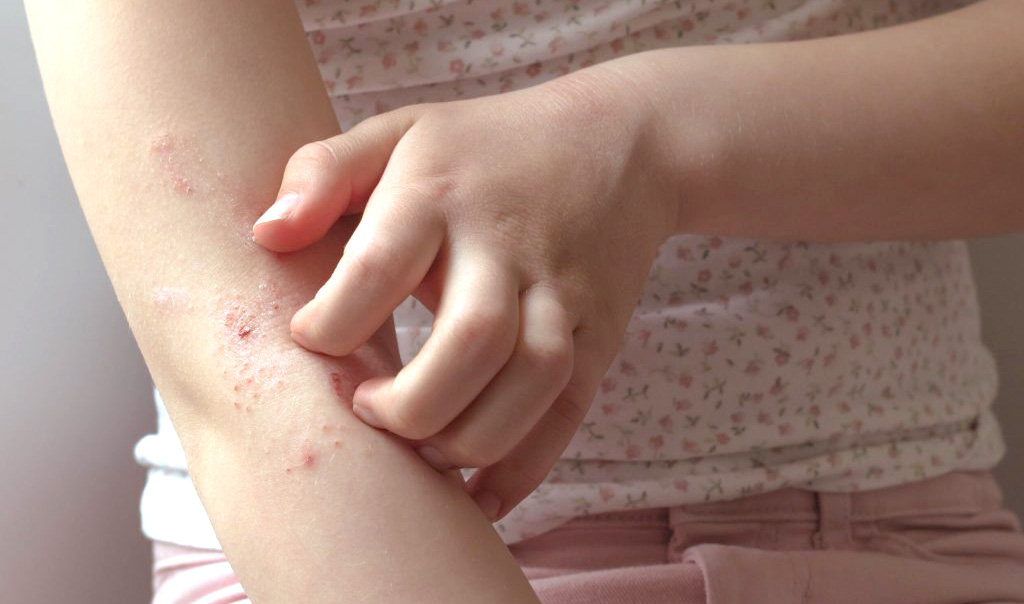
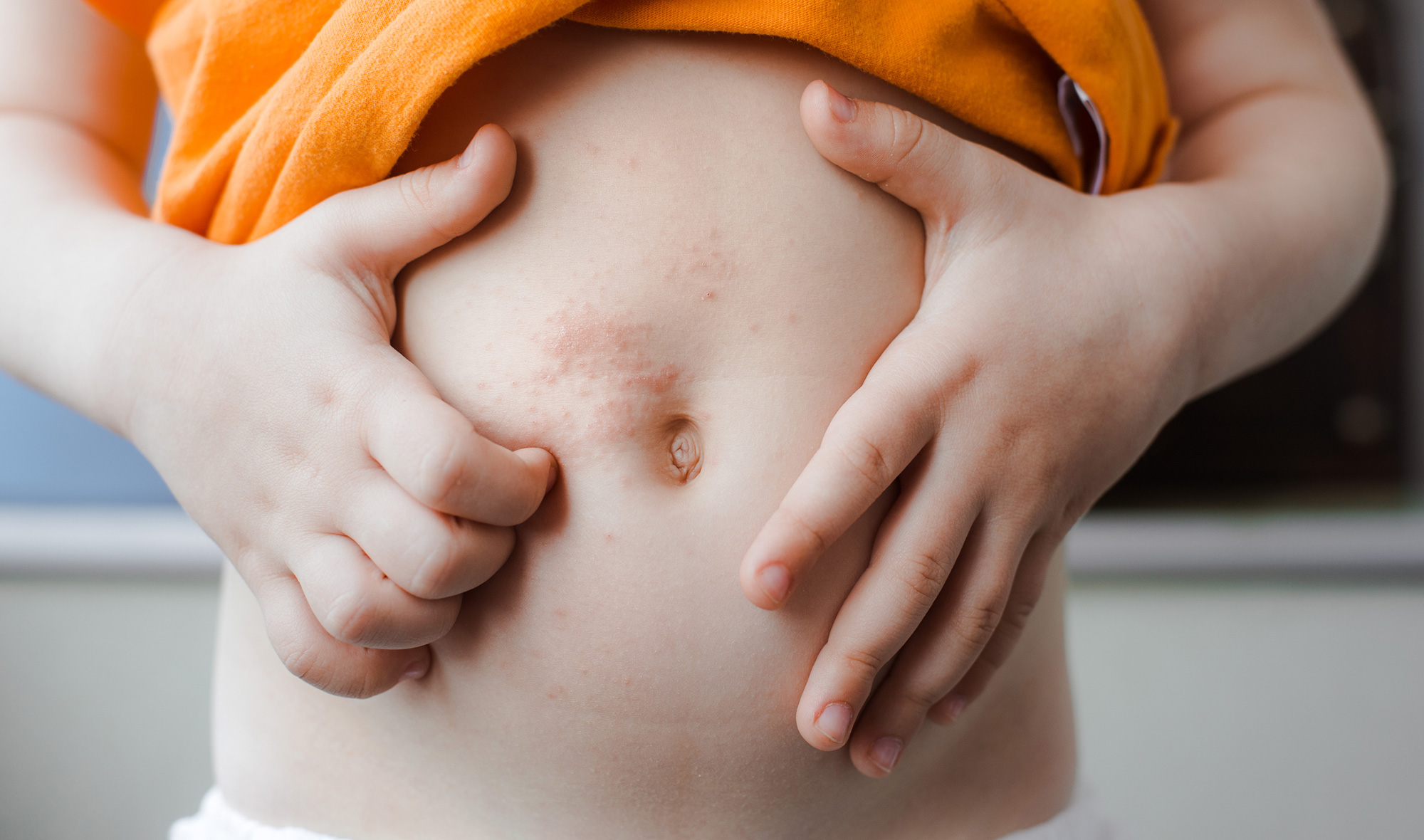
- Eczema or atopic dermatitis is the most common form of dermatitis where there is very sensitive skin that itches easily from scratching and rubbing. It often runs in families and can recur many times, often in the same place. It is thought to be caused by an overactive immune response to environmental factors and is linked with hayfever and asthma. It often affects several members of a family. Another likely cause is a breakdown in the skin’s barrier function so that it dries out more readily. Stress, low humidity, high temperatures, contact with some clothing such as wool, and certain chemicals such as soap, disinfectants or chlorine in swimming pools, UV light (sunlight) and overheating can all exacerbate symptoms. Eczema is divided into the infantile variety (between 2 and 6 months), juvenile (after 12 months) and adult. The juvenile variety is very itchy, tends to be recurrent and occurs in the joint creases. In adults in occurs mainly on the hands and face.
- Contact irritant dermatitis is caused by a substance that irritates and damages the skin when in direct contact; the amount of damage done depends on the sensitivity of the skin. Irritants include chemicals, such as a detergent or solvent, soap, skin cream and some plants like poinsettia. Having eczema also makes you more susceptible to this form of dermatitis.
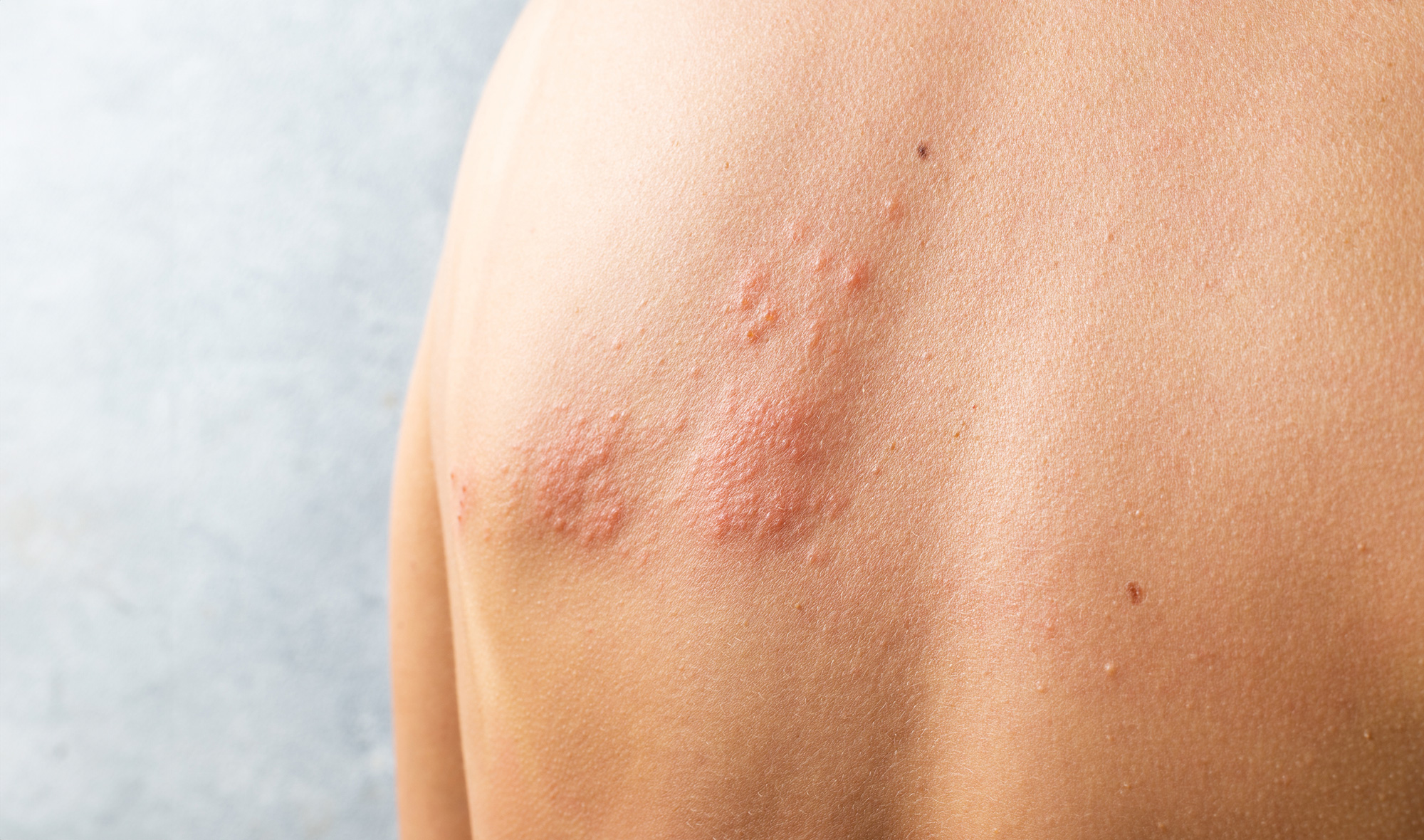
- Allergic contact dermatitis is caused by an immune reaction to a substance (allergen) in contact with the skin. Sensitisation is needed and this can be on the first exposure or after many exposures. Over time, the allergic response may get worse. Allergens include metal such as nickel or chrome found in jewellery, some plants such as the Rhus tree and poison ivy, perfume and latex rubber used to make gloves. Urushiol is a plant chemical found in poison ivy, poison oak, mango and cashew nuts and is a very common cause of allergic contact dermatitis.
- Seborrhoeic dermatitis causes mild to profuse skin flakes and scales on the scalp, face, eyebrows and lashes and around the nose and ears. In babies it is called cradle cap but is most common in middle age.
Prevention and treatment
Dermatitis is not infectious and once identified it can be treated.
1. Identify the cause
Unless you know the cause of your dermatitis it is difficult to treat, so finding the cause is important. Think about what you have been doing and where. Many cases of dermatitis are occupational, so consider work-related chemicals and latex gloves. Have you started using a new soap or washing powder? Does it occur after working in the garden? If you suspect a cosmetic or a perfume, test it on another area of skin and see if you get the same response. The location of the rash on your body may provide a clue to its cause, such as under a watch strap containing chrome or nickel – a common culprit.
2. Avoid the source
If you are able to identify the problem, try to avoid it. Change the brand or use a soap-free cleanser. Remove yourself physically where possible; if not, wear protective clothing, such as gloves or use a barrier cream. If you accidentally make contact with the problem substance, wash it off immediately after contact. Avoid dry skin by keeping water contact to a minimum and avoiding soap and detergents. Apply creams and ointments containing oil – these are better than lotions that are more water based. Clothing is important, avoid rough and synthetic fabrics and look out for central heating in winter.
3. Skin testing
If identifying the cause of your dermatitis is proving difficult consult your medical practitioner who may refer you for a patch test. This involves applying a range of substances directly to the skin under a piece of tape or gauze and then looking for a reaction after 48 hours, or longer, depending on the substance. Patch testing can be hit-and-miss and depends on the “right” allergen being tested.
4. Creams and ointments
- Barrier creams and moisturisers will help stop the skin drying out, allowing it to heal. Choose a basic cream with no additives or perfumes. An aqueous cream is always a good option as it is not greasy and available in bulk.
- Topical steroid creams and ointments (corticosteroids) are the mainstay of treatment and reduce the inflammation and therefore improve symptoms. You can get a low-dose cream without prescription, but for more concentrated topical steroids you will need to see your doctor.
- Antihistamines can be taken orally or topically (applied to skin) to help with itching.
- Aloe Vera is a plant extract known to have soothing properties, which you can buy as a gel from your pharmacy.
- Natural products such as manuka honey and tea-tree oil may help.
- It is impossible to overlubricate your skin.
5. Manage your dermatitis
Dermatitis, particularly eczema, can be a long-term problem, so it is important to manage it in your daily life. Look after your skin, keep it moisturised and avoid known irritants or allergens, where possible. Always be vigilant so that you can recognise and treat symptoms as soon as they appear, to prevent them worsening and risking infection. You may wish to try an alternative approach such as visit a naturopath, who will discuss your diet and lifestyle to address any issues you may not have uncovered before.













Community