What is Arthritis?
Arthritis is the major cause of disability in New Zealand and affects half a million people at some point in their lives, with more women than men affected. It is a chronic (long-term) disease and comes in many different forms, the most common being the degenerative Osteoarthritis (OA), which usually occurs later in life. Rheumatoid Arthritis (RA), which is a lot less common, can occur at any age but usually develops in younger people, even in young children, when it is known as juvenile arthritis; There are many other types of arthritis such as gout, where crystals of uric acid (a product of protein digestion) are deposited in bone, and ankylosing spondylitis, where the spine is inflamed and painful between the vertebrae.
What Causes Arthritis?
OA is caused by degeneration of the joint cartilage (the protective surface of the joint). This can happen either through aging, if a joint is put under excessive strain (such as long-term obesity), or if a joint is damaged by injury, especially fractures. The cartilage, which protects joints by acting as a shock absorber, gets worn away and the bones become irregular in shape and sometimes form outgrowths on their surface, causing bones to grind over each other – painfully. This usually happens in larger joints like the hip and shoulder but is also found in the vertebrae and bones of the hands and feet.
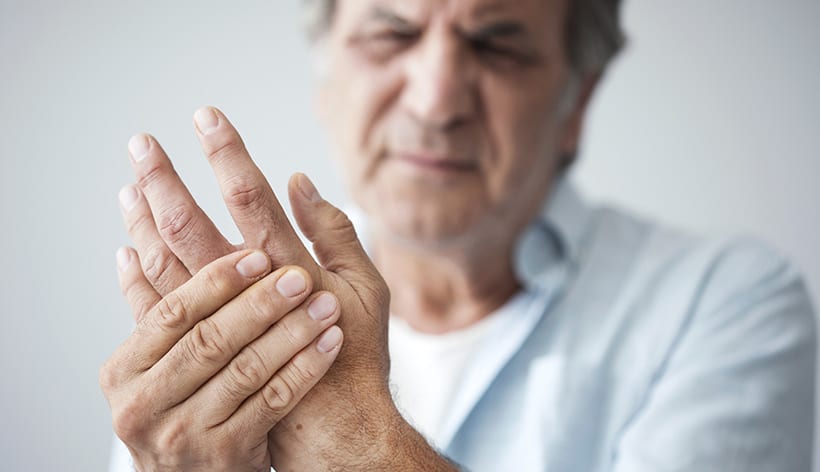
RA is an autoimmune disease which means that your immune cells attack your own joint tissues, affecting mainly small joints like fingers, wrists, elbows and ankles. The synovial membrane, which covers the ends of the bones, becomes inflamed and this leads to destruction of bone and cartilage leaving the joint severely damaged, swollen and painful.
Who Gets Arthritis?
There is a genetic predisposition for both forms of arthritis and if you have a family history of either OA or RA you are more likely also to develop arthritis. However, there is no evidence for specific inherited genes for arthritis. Being overweight is also a risk factor.
Symptoms
- Pain and stiffness in a joint
- Swelling around the joint caused by inflammation and increased fluid in the joint space
- Bony growths on the fingers (OA)
- Deformed and misshapen fingers (RA)
- Flu-like symptoms such as aching and fatigue (RA)
- A cracking sound or grating feeling as the joint moves (known as crepitus).
Prevention and Treatment
There is no cure for arthritis and it cannot be prevented, but there is a lot you can do to manage the disease. There are also ways you can reduce your risk of developing arthritis as well as control its progression.
Reduce your risk by healthy lifestyle
Being overweight puts strain on the joints, so keeping your weight within a healthy range will help maintain healthy bones. You can also keep your joints strong with exercise, good nutrition and by Including enough calcium and vitamin D in your diet.
Recognise symptoms and seek diagnosis
If you suspect you may have arthritis you don’t have to just put up with it. Early diagnosis is important especially if you are young and it is a sudden onset. Consult with your GP who may need to perform investigations such as:
- X-ray
- A blood test to identify conditions such as rheumatoid arthritis, gout and other inflammatory arthritis.
Keep symptoms at bay
There is no medication to prevent or cure arthritis, but there are several ways to ease the symptoms.
- Paracetamol is effective for pain relief, although it does not help with inflammation.
- A group of drugs called non-steroidal anti-inflammatory drugs (NSAIDs), have been widely used to help with joint pain. They work by reducing inflammation, but can cause irritation of the stomach. A newer group of NSAIDs, called COX-2 inhibitors have a lower incidence of stomach problems, but a higher risk of heart disease. It is best to discuss the pros and cons of using these drugs with your doctor.
- If you feel you need more effective pain relief, especially for inflamed joints, there is the option of corticosteroid injections into the joint which will provide temporary relief usually for a few months. There is also a synthetic lubricant injection which will give temporary benefit, however it is costly.
- Disease-modifying anti-rheumatic drugs (DMARDS) are available for inflammatory arthritis such as rheumatoid and psoriatic arthritis. They slow down or suppress disease progress but may take several months before they begin to work. Newer drugs are slowly becoming available that block the actions of a specific chemical that promotes inflammation.
Keep mobile
Exercise is a key factor in managing your arthritis. It will strengthen bones and muscles, which will help you keep active and mobile and also reduce joint pain and stiffness. Physiotherapy will also strengthen muscles around damaged joints helping them work better.
Consider surgery
If the affected joint becomes so damaged and the pain becomes so severe that nothing else will help, then you may want to consider joint replacement surgery. This will remove the pain and give you back your mobility. Other surgical treatments include synovectomy, which removes the inflamed lining of a joint.













Community